A fingernail. A tree branch. The corner of a piece of paper. A contact lens that went in wrong. A grain of sand at exactly the wrong moment. A scratched cornea — what we call a corneal abrasion — can come from almost anywhere, and when it happens, the pain is immediate and surprisingly intense.
Your eye is watering uncontrollably. Light feels unbearable. There’s a sensation like something is still in there even though you can’t find anything. And you’re wondering: do I go to the ER? Urgent care? Wait it out? Put something in it?
I want to give you real answers to those questions — the kind you’d get if you called my office right now. Most corneal abrasions heal completely on their own within a few days. But how you care for the eye in those first 24-48 hours makes a significant difference in how quickly that happens, how much you suffer in the meantime, and whether you avoid complications.
Here’s what you need to know.
What Is a Corneal Abrasion?
Your cornea is the clear, dome-shaped front surface of your eye. It’s the first lens light passes through on its way to your retina, and it’s responsible for a significant portion of your eye’s focusing power. It’s also the most exposed tissue in your body — there’s no skin, no fat layer, and no bone protecting it from the outside world.
A corneal abrasion is a scratch, scrape, or gouge on the surface of the cornea. The outer layer of the cornea — called the epithelium — is made up of cells that are both delicate and remarkably resilient. When something disrupts those cells, whether by direct contact, a foreign object, or friction, the result is a corneal abrasion.
Common causes include:
- Fingernails (your own or a child’s — babies are a surprisingly common cause)
- Tree branches, twigs, or plant leaves
- Paper edges, cardboard, or packaging
- Contact lenses — especially if inserted or removed incorrectly, worn too long, or worn in dry conditions
- Rubbing your eyes too aggressively, especially with dry eyes or something already in the eye
- Foreign particles — sand, sawdust, metal shavings, dirt — that get trapped under the eyelid and scrape the surface with each blink
- Sports injuries and direct eye trauma
- Makeup brushes, mascara wands, and eyeliner applicators
Some people develop corneal abrasions without any obvious external cause, due to severe dry eye disease causing the eyelid to stick to the corneal surface during sleep. This is closely related to a condition called corneal erosion, which we’ll cover later in this article.
Symptoms: What a Scratched Cornea Feels Like
If you’ve had a corneal abrasion, you probably don’t need a list to recognize it. But here’s what to expect and watch for:
- A persistent sensation that something is in your eye — even after flushing thoroughly and finding nothing. This is the nerve endings responding to the damaged surface, not an actual foreign body.
- Significant pain — often disproportionate to how minor the original incident seemed
- Uncontrollable tearing — your eye’s reflex response to injury
- Light sensitivity (photophobia) — even normal indoor lighting can feel harsh and painful
- Blurred or hazy vision — the disrupted corneal surface scatters light rather than focusing it cleanly
- Redness — from irritation and increased blood flow to the eye surface
- Headache — often developing from squinting and light sensitivity
- Eyelid spasm — involuntary blinking or difficulty keeping the eye open
The severity of symptoms doesn’t always correlate with the size of the abrasion. Some very small scratches in highly sensitive areas of the cornea cause extreme pain, while larger abrasions in less innervated areas may feel milder.
Why Does a Scratched Cornea Hurt So Much?
The cornea has one of the highest concentrations of pain receptors — called nociceptors — of any tissue in the human body. There are hundreds of times more pain receptors per square millimeter in your cornea than in your skin. This is not a design flaw. It’s a protective mechanism: the extreme sensitivity of the cornea exists to alert you immediately when something is wrong, so you respond before serious damage occurs.
When the epithelium is disrupted, those nerve endings are exposed directly to the environment — to air, light, and the friction of every blink. That’s what makes a corneal abrasion so relentlessly uncomfortable. Your eye is not overreacting. It’s doing exactly what it’s supposed to do.
The good news: those same nerve endings facilitate remarkably fast healing. Corneal epithelial cells are among the fastest-regenerating cells in the body. A small abrasion can resurface completely within 24-48 hours.
What to Do Immediately After Scratching Your Eye
The first few minutes after a corneal abrasion matter. Here’s exactly what to do — and what not to do.
Do This:
- Rinse gently with clean water or sterile saline. If there’s a foreign object in the eye, this gives it the best chance of flushing out. Use a steady, gentle stream — a clean cup of water, a saline eyewash bottle, or an eye wash station if you’re at a workplace.
- Blink several times. Your tears are doing their job. Let them. Blinking can help dislodge a superficial foreign body.
- Pull your upper eyelid gently over your lower eyelid. The lashes of the lower lid may brush the inner surface of the upper lid and remove a particle.
- Call Eye Care Center. A corneal abrasion is an ocular emergency that warrants same-day evaluation. We can assess the injury, confirm the cause, prescribe appropriate treatment, and rule out complications.
Do Not Do This:
- Do not rub your eye. Rubbing is one of the worst things you can do with a corneal abrasion. It increases friction across damaged tissue, can drive a foreign body deeper, and significantly slows healing.
- Do not try to remove a foreign body with your finger, a cotton swab, or any other object. If something is embedded in the corneal surface, it requires professional removal under magnification.
- Do not wear contact lenses until you’ve been evaluated and cleared by your optometrist. A lens over an abrasion dramatically increases infection risk and interferes with healing.
- Do not use over-the-counter redness-relief eye drops (like Visine or Clear Eyes). These are vasoconstrictors that reduce surface redness but have no role in healing a corneal abrasion and may cause further irritation.
- Do not patch your eye without being instructed to by a doctor. Current evidence suggests that eye patches do not speed healing and may actually slow it for most types of corneal abrasions.
Can Urgent Care Treat a Scratched Cornea?
This is one of the most common questions we hear — and it’s a fair one, especially if your abrasion happens on a weekend evening or you’re unsure whether it’s serious enough for a dedicated eye care visit.
The short answer: urgent care can help in a pinch, but an optometrist is significantly better equipped to evaluate and treat your eye.
Here’s the practical reality. Urgent care physicians are generalists. They can confirm that your eye is red and painful, prescribe antibiotic drops, and advise you not to rub it. That’s valuable — and better than nothing — but it represents only part of what a comprehensive eye evaluation actually involves.
What urgent care typically cannot do:
- Examine your cornea under high magnification with a slit lamp to assess the size, depth, and exact location of the abrasion
- Use fluorescein dye to precisely map the abrasion and rule out deeper corneal involvement
- Check intraocular pressure, which can be affected by certain types of eye trauma
- Assess your retina for trauma-related changes — especially important after direct blunt impact to the eye
- Identify whether a foreign body remains embedded in the corneal tissue
- Remove an embedded foreign body safely
- Fit a bandage contact lens to reduce pain and facilitate faster healing
- Recognize the signs of a more serious underlying condition mimicking a simple abrasion
An emergency room is appropriate for trauma involving possible penetrating injury, significant vision loss, chemical burns with large-volume exposure, or injuries where there is concern about damage beyond the surface of the eye. For a standard corneal abrasion from a fingernail, contact lens, or small foreign body, Eye Care Center is the right place to go — and we’ll see you the same day.
We have the diagnostic equipment, the training, and the clinical context of your eye history to give you a thorough evaluation and the most appropriate treatment. That’s simply a different level of care than a generalist urgent care visit provides.
Call any of our locations in Addison, Burbank, or Willowbrook and let us know what happened. We will fit you in.
How Corneal Abrasions Are Treated
When you come in with a suspected corneal abrasion, here’s exactly what happens at Eye Care Center.
Diagnosis
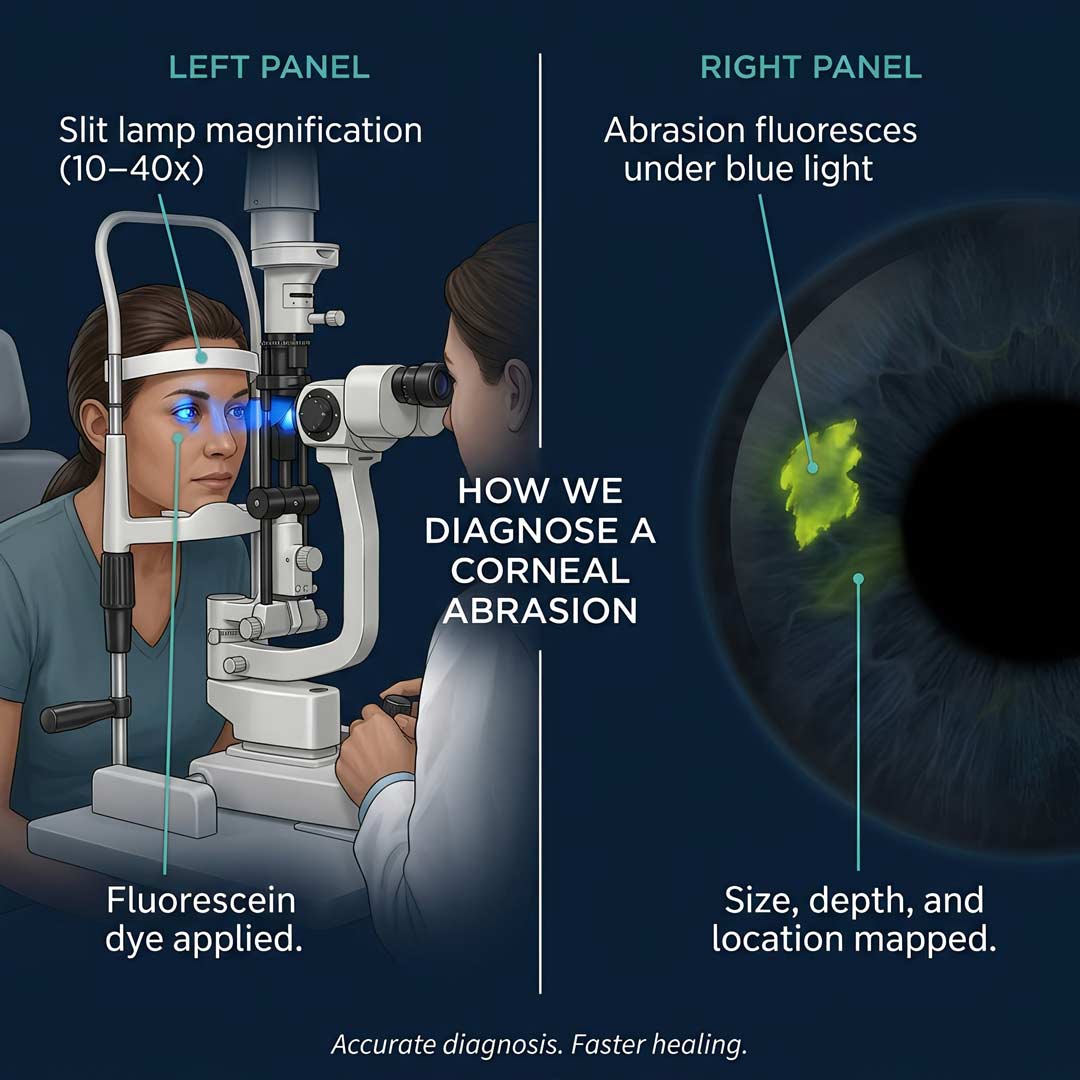
We’ll start with a brief history — what happened, when, and what your symptoms have been since. Then we’ll examine your eye under the slit lamp, a binocular microscope that lets us see your cornea at 10 to 40 times magnification.
We’ll apply a drop of fluorescein — a safe, temporary orange dye — to the surface of your eye. Under blue light, the dye fluoresces a vivid yellow-green anywhere the corneal epithelium has been disrupted. This gives us a precise map of the abrasion: its size, its location on the cornea, and whether it extends into deeper corneal layers.
We’ll also examine the underside of your eyelid to check for a retained foreign body — a particle that may still be there even after flushing. This is one of the most common things urgent care physicians miss, because it requires everting (flipping) the eyelid and examining it under magnification.
Treatment Options
Treatment depends on the size and location of the abrasion, whether a foreign body is involved, and your overall eye health. Here’s what we may recommend:
Antibiotic eye drops or ointment: The corneal surface is an entry point for infection. We prescribe topical antibiotics not because your abrasion is infected, but to prevent infection while the epithelium is open and healing. This is standard care for virtually all corneal abrasions.
Lubricating drops or ointment: A thick lubricating ointment at night serves two purposes: it keeps the corneal surface moist to facilitate healing, and it reduces the friction of the eyelid moving across the damaged surface while you sleep. Preservative-free lubricating drops during the day provide similar relief with less blur.
Dilating drops: For moderate to severe abrasions, we may prescribe a dilating drop. This relaxes the ciliary muscle inside the eye — a muscle that goes into painful spasm when the cornea is significantly injured. Dilation doesn’t heal the abrasion, but it substantially reduces the deep aching pain that accompanies more serious injuries.
Bandage contact lens: For larger or more painful abrasions, a soft bandage contact lens can be placed over the cornea. The lens acts as a physical barrier between the raw corneal surface and the friction of the blinking eyelid. Many patients experience dramatic pain relief within minutes of having a bandage lens placed. We’ll monitor you closely while you have it in and remove it once healing is confirmed.
Foreign body removal: If a particle remains embedded in the corneal tissue, we’ll remove it using a fine instrument or a specialized ophthalmic burr — a procedure that sounds alarming but is performed with topical anesthetic drops and takes only a few minutes.
Eye patch: Patching fell out of favor as primary treatment for most corneal abrasions after studies showed it didn’t improve healing speed and left patients more uncomfortable. We rarely recommend it for standard abrasions, though there are specific circumstances where it’s still appropriate.
Eye Drops for Corneal Abrasion: What Actually Helps
Patients often arrive having already tried something from the medicine cabinet. Let me be direct about what helps and what doesn’t.
What Helps
Preservative-free artificial tears — lubricating drops labeled “preservative-free” (look for unit-dose vials or bottles specifically labeled as such) are appropriate for comfort while you wait to be seen. They keep the surface moist without interfering with healing. Use as often as needed.
What Does Not Help (And May Make Things Worse)
Redness-relief drops (Visine, Clear Eyes, and similar products): These work by constricting surface blood vessels to reduce the appearance of redness. They do nothing to address corneal healing and can cause rebound redness with repeated use. Avoid these entirely.
Numbing drops (proparacaine, tetracaine): These are ophthalmic anesthetics that eye doctors use diagnostically and for procedures. They are not for home use. Topical anesthetics feel miraculous on a painful abrasion — and that’s exactly the problem. They eliminate the pain signal that tells you not to rub the eye, and with repeated application, they significantly impair corneal healing and can cause serious, permanent corneal toxicity. If you have access to these drops at home from a previous prescription, do not use them on a fresh abrasion.
Antibiotic drops from an old prescription: Resist the temptation. The antibiotic may not be the right one for your current situation, the drop may be expired, and some older antibiotic formulations can be irritating to an already-damaged surface. Let us prescribe the right medication for what we actually find in your eye.
The appropriate drops — antibiotic and lubricating — will be prescribed at your visit based on what we observe. There is no over-the-counter equivalent to the treatment plan we’ll put together after examining your eye.
How Long Does a Scratched Cornea Take to Heal?
The corneal epithelium heals faster than almost any other tissue in the body. For most patients:
- Small abrasions (a fingernail nick, paper edge, small particle): 24-48 hours for surface closure, with significant pain improvement often within the first day
- Moderate abrasions: 2-4 days for surface healing; some residual light sensitivity may linger briefly
- Large or deep abrasions: up to 1 week, and in some cases follow-up evaluation is important to ensure complete healing without complications
A few things that slow healing:
- Rubbing or touching the eye during recovery
- Returning to contact lens wear before the eye is fully healed
- Existing dry eye disease, which compromises the tear film that facilitates epithelial repair
- Retained foreign body that wasn’t identified and removed
- Infection developing in the healing tissue
If your pain is significantly worsening after 48 hours — rather than improving — or if you develop increasing redness, discharge, or notable vision change, contact us immediately. These can be signs that an infection is developing, which requires prompt treatment. Learn more about why eye health monitoring matters in our comprehensive exam guide.
Corneal Erosion: When the Problem Comes Back
Some patients who’ve had a corneal abrasion go on to develop a related condition called recurrent corneal erosion (RCE). This happens when the epithelial cells that replaced the original injury don’t bond as strongly to the underlying layer — called Bowman’s membrane — as healthy cells do.
The result: the new cells lift or tear away, often at the most inconvenient possible moment. Many patients describe waking up with sudden, severe eye pain that feels identical to their original abrasion — sometimes months after the initial injury seemed fully healed. The mechanism makes sense: your eyes become very dry during sleep, and the eyelid can adhere to a weakly attached epithelium. Opening your eyes in the morning creates a tearing force across that fragile junction.
Risk factors for corneal erosion include:
- A prior corneal abrasion (especially from a fingernail, plant material, or paper)
- Chronic dry eye disease
- Corneal dystrophies (inherited structural conditions affecting the cornea)
- Improper contact lens fit or care
Treatment for recurrent erosion follows the same initial steps as a standard abrasion, but if erosions recur two or more times, more definitive treatment becomes appropriate. Options include:
- Nightly hypertonic saline ointment (sodium chloride 5%) to draw excess fluid from the epithelium and strengthen adhesion
- Extended bandage contact lens wear under close monitoring
- Anterior stromal puncture — a minor procedure that creates tiny anchor points to help the epithelium bond more securely
- Superficial keratectomy or excimer laser (PTK) — removing the irregular epithelium to allow a healthier regrowth
If you’re experiencing what sounds like corneal erosion — especially waking pain that comes and goes — don’t assume it will resolve on its own. Let us evaluate your corneal surface and map out the right management plan for you.
How to Prevent a Scratched Cornea
Most corneal abrasions are genuinely preventable. The habits that protect your cornea overlap significantly with general eye safety practices — all of which we cover in detail in our complete eye safety guide.
The highest-yield habits for corneal protection specifically:
- Wear appropriate protective eyewear for any task involving tools, debris, chemicals, or high-velocity particles. ANSI Z87.1-rated safety glasses provide corneal protection that standard prescription lenses simply do not.
- Keep your fingernails trimmed — both yours and your children’s. Baby and toddler nails are responsible for a meaningful number of the corneal abrasions we see, because children move unpredictably near your face and their nails are sharper than you’d expect.
- Follow contact lens wear and care protocols carefully. Many contact lens-related abrasions result from lenses worn too long (causing a tight lens syndrome on removal), inserted with debris on the lens surface, or handled with dry fingers. Our full contact lens safety guide covers this in detail.
- Be careful with eye makeup — mascara wands, eyeliner pencils, and makeup brushes near an open eye require a steady hand and good lighting. Never apply eye makeup in a moving vehicle.
- Manage dry eye disease. Chronic dry eye creates a compromised tear film that allows the eyelid to drag more aggressively across the corneal surface — increasing both abrasion and erosion risk. Read about dry eye treatment options we offer.
- Wear sports goggles for any contact sport or ball sport. A direct hit to the unprotected eye — from a ball, elbow, or finger — is one of the more serious mechanisms of corneal injury we see.
Frequently Asked Questions: Corneal Abrasions
Can a scratched cornea heal on its own?
Small to moderate corneal abrasions will often heal on their own within 1-3 days, because corneal epithelial cells regenerate faster than almost any other cell in the body. However, “healing on its own” doesn’t mean you should skip evaluation. An untreated abrasion carries real risks: a retained foreign body that wasn’t identified, an infection developing in the healing tissue, or a deeper injury that requires different management. Getting evaluated within 24 hours lets us confirm what we’re dealing with, prescribe the right treatment to help you heal faster and more comfortably, and rule out complications before they become more serious.
Can urgent care treat a scratched cornea?
Urgent care can provide basic care — typically antibiotic drops and instructions to rest the eye — but it is not the ideal setting for corneal abrasion management. Urgent care facilities generally do not have slit lamps, fluorescein staining capability, or the equipment to safely remove a retained foreign body from the corneal surface. An optometrist has the training, equipment, and clinical context to give you a complete evaluation. Eye Care Center will see you the same day for corneal injuries at our Addison, Burbank, and Willowbrook locations. Call us before defaulting to urgent care for any eye injury.
What eye drops are safe to use for a corneal abrasion?
Preservative-free artificial tears are safe and appropriate for comfort while you wait to be seen. Avoid redness-relief drops (Visine, Clear Eyes), which won’t help healing. Never use numbing drops (anesthetics) at home — they feel helpful immediately but impair healing and can cause serious corneal damage with repeated use. The appropriate antibiotics and lubricants will be prescribed after your evaluation.
How long does a scratched cornea take to heal?
Small abrasions typically close within 24-48 hours. Moderate abrasions generally heal in 2-4 days. Larger or deeper injuries may take up to a week. Pain should be improving by day two. If your pain is getting significantly worse rather than better after 48 hours, contact us — this may indicate an infection or complication requiring prompt treatment.
Should I patch my eye after a corneal abrasion?
Current evidence does not support eye patching as a routine treatment for most corneal abrasions. Clinical studies have shown that patching generally does not accelerate healing and may leave patients more uncomfortable. There are specific situations where we may recommend a patch, but this should be a physician’s decision based on examination findings — not something to do at home based on instinct.
Can I wear contacts after a corneal abrasion?
No — not until you’ve been cleared by your optometrist. A contact lens over a healing corneal abrasion significantly increases the risk of infection, which can be serious and far more complicated to treat than the original abrasion. Many patients can return to lenses within a few days of a small abrasion, but the timing depends on how completely the epithelium has healed. We’ll tell you exactly when it’s safe to go back.
I got poked in the eye and my vision went blurry. Is that normal?
Some temporary blur is common with corneal abrasions because the disrupted surface scatters light. This usually improves as the cornea heals. However, significant or persistent vision loss after any eye trauma — especially blunt force — warrants immediate evaluation. Beyond the cornea, a poke or impact can affect the lens, cause bleeding inside the eye, or create retinal changes that are not apparent from the outside. If your vision is notably worse or doesn’t improve, don’t wait. Sudden new floaters or flashes of light after eye trauma are also red flags that require same-day evaluation.
What’s the difference between a corneal abrasion and a corneal erosion?
A corneal abrasion is an acute injury — a scratch or scrape caused by an identifiable event. Corneal erosion is a recurrence that happens when the cells that healed an original abrasion don’t bond securely to the layer beneath them. Erosion typically presents as sudden, severe eye pain that starts on waking, without any obvious new injury. It’s the same surface disruption, but caused by the eyelid peeling away weakly attached cells rather than an external event. Recurrent erosion can be managed, and in some cases treated definitively, with procedures we offer at Eye Care Center.
A scratched cornea is one of the most common eye emergencies we see — and one of the most treatable when you get proper care promptly. If you’re dealing with eye pain, light sensitivity, or the sensation that something is in your eye, don’t wait it out.
Eye Care Center LTD sees same-day urgent eye care patients at all three locations: Addison, Burbank, and Willowbrook.
Book online or call us at 1-888-899-0816. We’ll take care of your eye.