Your Eye Exam Is Not a Vision Test. Here’s What Your Eye Doctor Is Actually Looking For.
Think your eye exam is just about glasses? Dr. Park reveals what’s really happening, including the diseases being caught before you notice a single symptom.
By Dr. Quentin Park, O.D. | The Eye Care Center, serving Addison, Burbank & Willowbrook, Illinois
I want to tell you about a patient I saw last year. She came in for a routine exam, nothing dramatic, just an annual check, maybe a prescription update. She felt fine. Her vision seemed about the same. What I found during her dilated fundus exam told a very different story: early diabetic retinopathy in both eyes. She had no idea she had diabetes. No diagnosis, no symptoms, no warning she had ever received. We referred her to her primary care physician the same day. She started treatment within the week. Her vision today is intact because she kept an appointment she almost cancelled.
That story is not unusual in my practice. It happens more often than most patients would expect, and it happens because of a fundamental misunderstanding about what a comprehensive eye exam actually is. Most people walk into one of our offices in Addison, Burbank, or Willowbrook expecting something close to the vision screening they remember from school: read some letters, confirm your prescription, pick out frames. What they get instead is one of the most information-dense health evaluations available in primary care. I am examining your blood vessels, your optic nerve, your retinal layers in cross-section, the pressure inside your eye, the surface of your cornea in three dimensions, and the clarity of your lens. I am looking for over 270 conditions, the majority of which produce zero symptoms in their early stages. Your prescription? That is maybe 20% of what we are doing.
This article is my attempt to pull back the curtain completely. I am going to walk you through every component of a comprehensive eye exam, covering what we are doing, what we are looking for, and why it matters for your long-term health in ways that extend well beyond your ability to read a highway sign. By the end, I hope you will never think about an annual eye exam the same way again.
Your eyes are the only place in the human body where blood vessels, nerve tissue, and central nervous system tissue can be directly visualized without surgery or invasive procedures. During a comprehensive eye exam, I can detect signs of diabetes, hypertension, multiple sclerosis, brain tumors, stroke, certain cancers, and over 270 other conditions, most of them before a single symptom has appeared anywhere in your body.
– Dr. Quentin Park, O.D. | The Eye Care Center
Your Eye Exam Is a Full-Body Health Screening (And You Didn’t Even Know It)
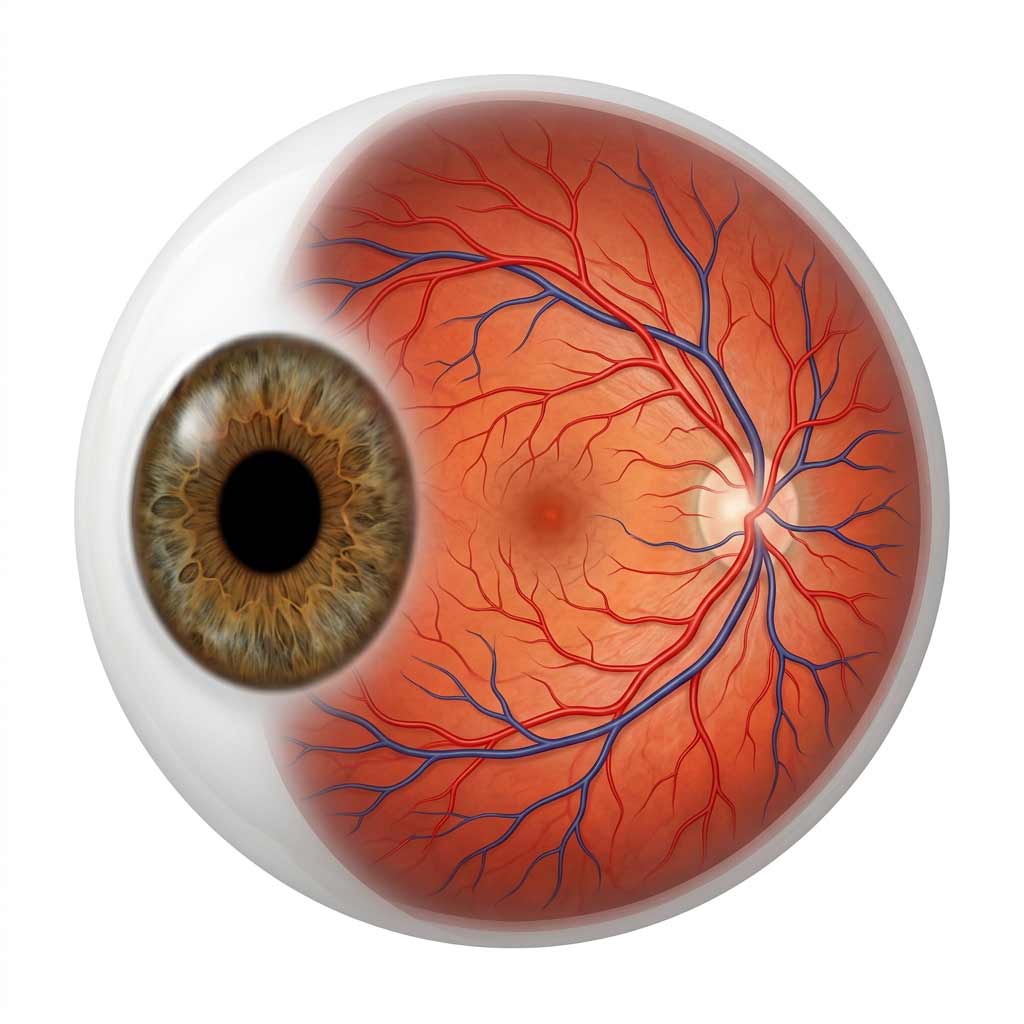
The anatomical fact that makes a comprehensive eye exam uniquely powerful in preventive health care is this: your eyes are the only location in your entire body where blood vessels, nerve tissue, and central nervous system tissue can be examined directly, in real time, without a single incision or invasive instrument. Every other organ system requires imaging, blood work, or surgical access to visualize at this level of detail. Your retina offers it with a light source and a lens.
When I look through an ophthalmoscope or review an OCT scan of your retina, I am not looking at an approximation of your vascular and neurological health. I am looking at the actual tissue. The tiny arteries and veins crossing your retinal surface reflect the condition of your cardiovascular system directly: narrowing, thickening, arteriovenous nicking, flame-shaped hemorrhages: these are the retinal signatures of hypertension, atherosclerosis, and stroke risk. The optic nerve, visible from the front of the eye, is a direct extension of your brain, and changes in its appearance, specifically cupping, pallor, and swelling, can signal glaucoma, elevated intracranial pressure, or neurological disease. The retinal tissue itself is metabolically demanding, and it is often among the first tissues in the body to show the vascular damage of uncontrolled diabetes.
Over the course of my career, I have detected undiagnosed Type 2 diabetes in patients who came in for nothing more than an updated prescription. I have found papilledema, which is swelling of the optic nerve from elevated intracranial pressure, in a patient who had been experiencing headaches that had not yet prompted a neurological workup. I have identified hypertension in patients with no primary care relationship. These are not dramatic exceptions. They are the natural result of what a comprehensive eye exam, performed thoroughly and with appropriate technology, is capable of finding. The systemic conditions we actively screen for alongside eye-specific disease include diabetes and pre-diabetes, hypertension, autoimmune conditions including rheumatoid arthritis, lupus, and multiple sclerosis, thyroid disorders, elevated cholesterol, neurological conditions and brain tumors, and certain cancers including leukemia, lymphoma, and ocular melanoma. Most of these conditions have no symptoms in early stages. The eye exam, for many patients, is the first clinical encounter where evidence of them appears.
What Happens During Each Part of Your Exam
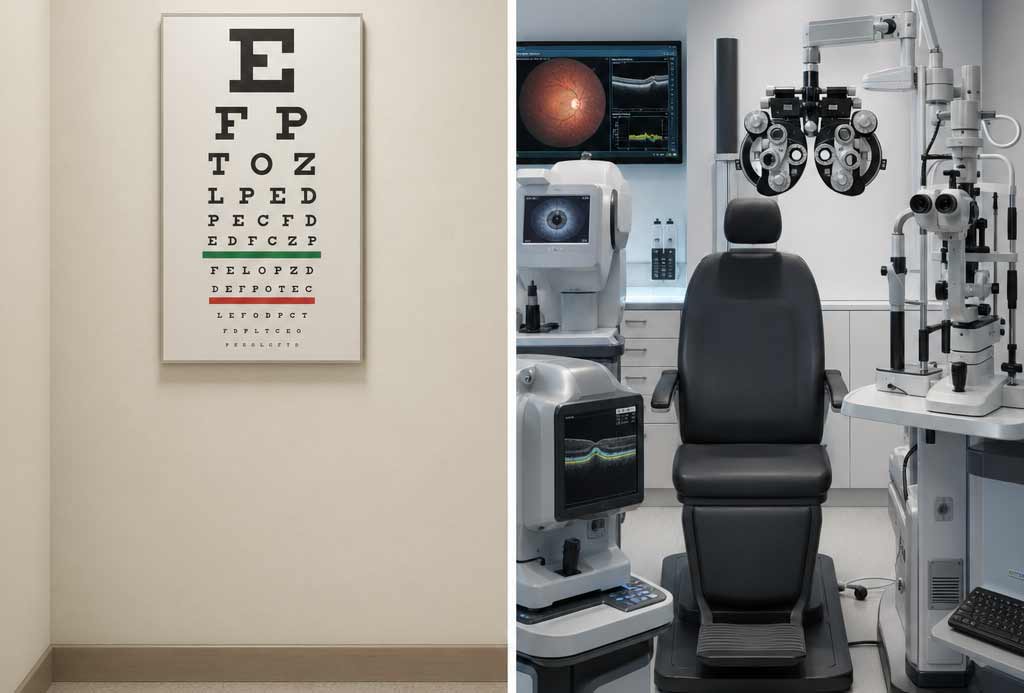
A comprehensive eye exam at any of our three locations runs between 45 and 90 minutes, depending on whether advanced imaging is indicated. Here is exactly what we are doing at each stage and why each component matters.
We start with patient history, and I want to be clear that this is not administrative paperwork. It is clinical detective work. Your current symptoms, medical history, medications, family history of eye disease, and lifestyle all shape what I am looking for during the exam. Many medications affect the eyes in ways patients do not expect: steroids can accelerate cataract formation and raise eye pressure; antihistamines reduce tear production and worsen dry eye; blood pressure medications can affect retinal blood flow. Family history of glaucoma doubles your lifetime risk. None of this information reaches me unless I ask, and the exam I perform changes meaningfully based on what I learn.
Visual acuity testing follows. The letter chart which most people recognize as the exam. We test distance vision, near vision, each eye separately, and compare corrected to uncorrected performance. The pattern here matters as much as the result. Sudden vision loss in one eye is a potential emergency. Gradual bilateral blur is probably a refractive change. An eye that is significantly worse than it was last year, or significantly worse than the other eye, flags a follow-up investigation. The chart is not just about your prescription. It is about tracking change over time.
Refraction, the “which is better, one or two?” portion, determines your optimal lens prescription across sphere power, cylinder power, and axis. We are also evaluating binocular balance, ensuring both eyes are working together rather than one eye compensating for the other in ways that cause fatigue or headaches. Then comes eye movement and alignment testing: extraocular motility, pupil responses, cover test for muscle imbalance, and convergence. Problems here cause double vision, reading difficulties, and headaches, particularly in children, where a muscle imbalance can be silently affecting reading comprehension and classroom performance for years before anyone connects the symptom to its source.
Intraocular pressure measurement, using either the air puff or the applanation tonometry if we need the gold standard, measures the pressure inside your eye. Normal range is 10 to 21 mmHg, but I am not just looking at absolute numbers. I am looking at asymmetry between eyes and trends over time. A patient at 19 mmHg this year who was at 14 last year deserves a closer look at their optic nerve, even if both numbers are technically within normal range.
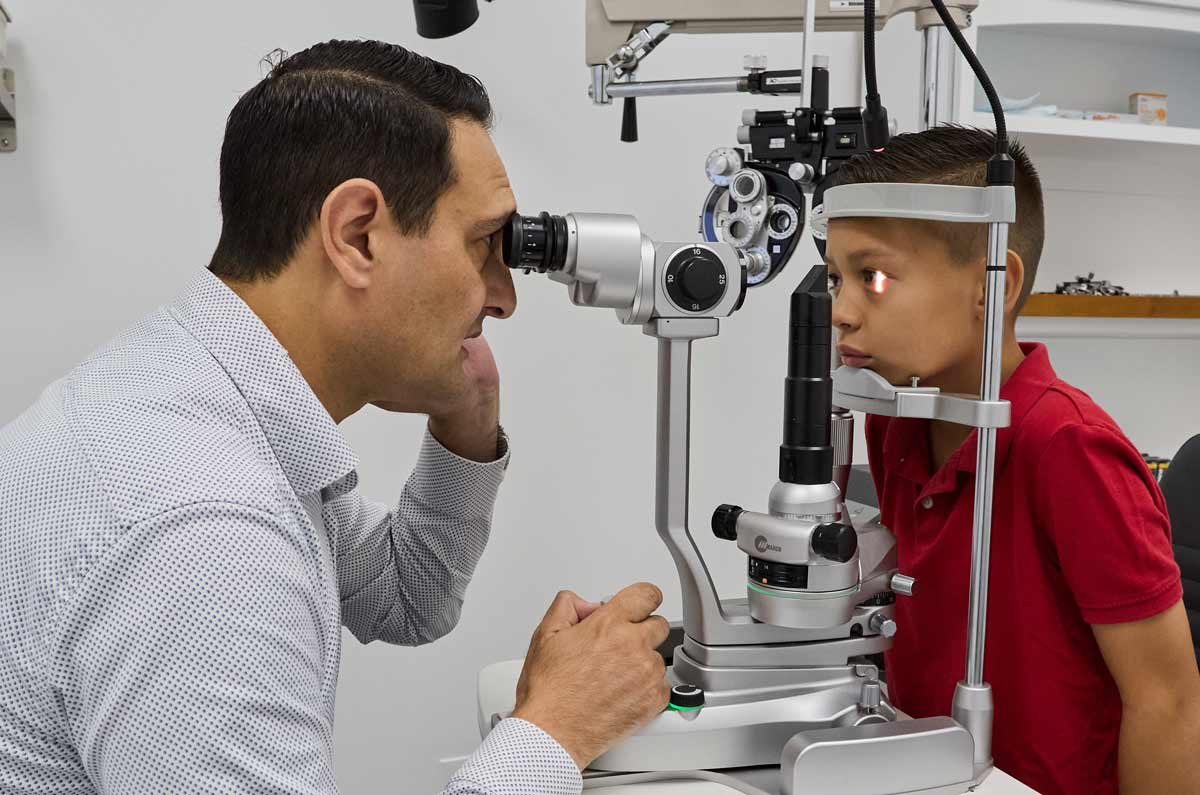
The slit lamp examination is where I examine your eyes under microscopy at 10 to 40 times magnification, evaluating your eyelids and lashes, the conjunctiva, the corneal surface, the anterior chamber, the iris, and the lens. I can see individual cells at this level. I can measure tear film breakup time to quantify dry eye disease. I can identify early cataract formation years before it affects your vision, and grade its density to help us plan timing of any future intervention. Meibomian gland dysfunction, the most common driver of evaporative dry eye, is visible at the lid margin. Corneal scars, infections, and dystrophies are all part of the slit lamp picture.
The dilated fundus examination is, in my view, the most important component, and the one patients are most likely to decline because the dilation drops are inconvenient. Please do not decline it. Without dilation, I can visualize approximately 30 to 40% of your retina. With dilation, I see 90 to 95%. The difference between those two numbers is the difference between catching a peripheral retinal tear before it becomes a detachment and missing it entirely. After the drops take effect, I am examining your optic nerve for signs of glaucoma, cupping, or atrophy; the macula for drusen, fluid, hemorrhage, or the early signs of macular degeneration; the retinal blood vessels for diabetic or hypertensive changes; the peripheral retina for tears, lattice degeneration, and detachment; and the vitreous for hemorrhage or inflammation. This part of the exam is irreplaceable. No imaging technology we have, however good, fully substitutes for a dilated clinical examination by an experienced clinician.
The Technology That Sees What Eyes Cannot
The clinical exam I described above is the foundation. The imaging technology we have at The Eye Care Center extends what is possible well beyond what any clinical eye can see alone.
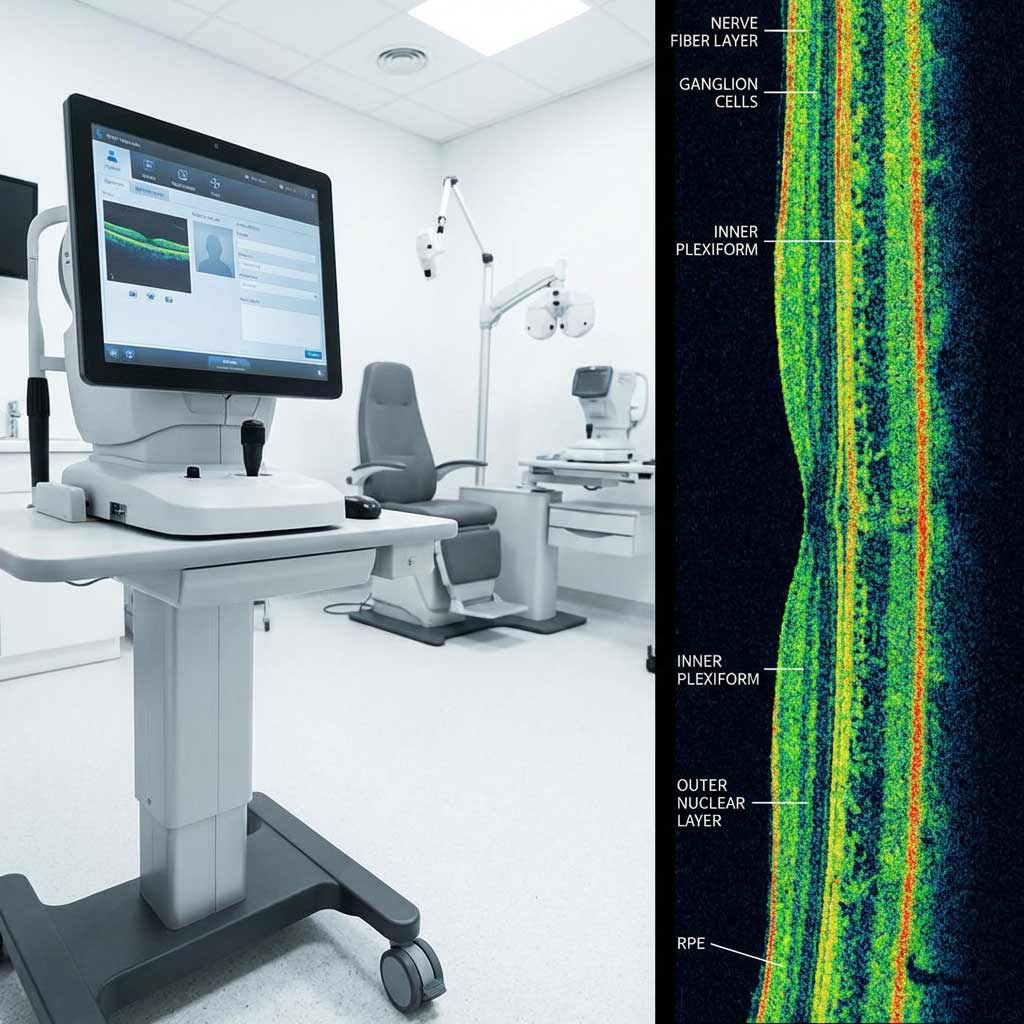
OCT (Optical Coherence Tomography) is the most significant advancement in diagnostic optometry in the past two decades, and I want to explain specifically why. OCT uses light waves to create cross-sectional images of your retinal layers at a resolution of approximately 5 microns, about one two-hundredth the thickness of a human hair. It is, in functional terms, an MRI for your eye, and it allows me to measure the thickness of individual retinal layers with precision that was not clinically available at all fifteen years ago. For glaucoma, this is transformative: I can detect measurable thinning of the nerve fiber layer five to ten years before it produces detectable visual field loss. That lead time is the difference between preserving functional vision and spending those years watching damage occur while waiting for symptoms. For macular degeneration, OCT detects fluid accumulation beneath the retinal pigment epithelium at a stage when treatment is most effective, before central vision has begun to distort. For diabetic macular edema, it quantifies retinal swelling with a precision that guides treatment decisions directly.
Retinal photography provides high-resolution color documentation of your retinal health that compounds in value over time. A single retinal photo tells me about today. A series of retinal photos taken annually tells me about trajectory. I have caught early macular degeneration by comparing this year’s photograph to last year’s and noticing drusen deposits that were barely visible but definitely growing. That kind of subtle longitudinal change is invisible without a documented comparison, and it is the reason I encourage patients to have retinal photography at every annual exam, not just when something looks suspicious.
Visual field testing maps your entire field of peripheral vision, meaning not just what you see straight ahead but everything detectable without moving your eyes. Glaucoma is the primary application: it creates characteristic and reproducible patterns of peripheral vision loss that are identifiable on visual field maps long before a patient notices any change in day-to-day vision. By the time a glaucoma patient notices peripheral vision loss on their own, they have typically already lost 40 to 50% of their peripheral visual field, a loss that is not reversible. Visual field testing also detects patterns associated with brain tumors, stroke, retinal detachment, and neurological disease, based on the anatomical correlation between where vision loss appears on the map and where in the visual pathway the damage is located.
Corneal topography creates a detailed three-dimensional map of your corneal surface, essential for specialty contact lens fitting, pre-surgical refractive evaluation, and the detection of keratoconus, a progressive corneal thinning disease that causes irregular astigmatism and vision distortion. We have identified early keratoconus in teenage patients whose routine prescription was changing in ways that suggested something other than standard myopia progression, and referred them for corneal cross-linking, a procedure that halts the disease’s progression when caught early. Without topography, those patients would have continued to receive updated glasses prescriptions while the underlying corneal condition progressed unchecked.
The Conditions That Have No Symptoms, Until They Do
Let me walk through the conditions I am most actively looking for and why the timing of detection matters so profoundly for each one.
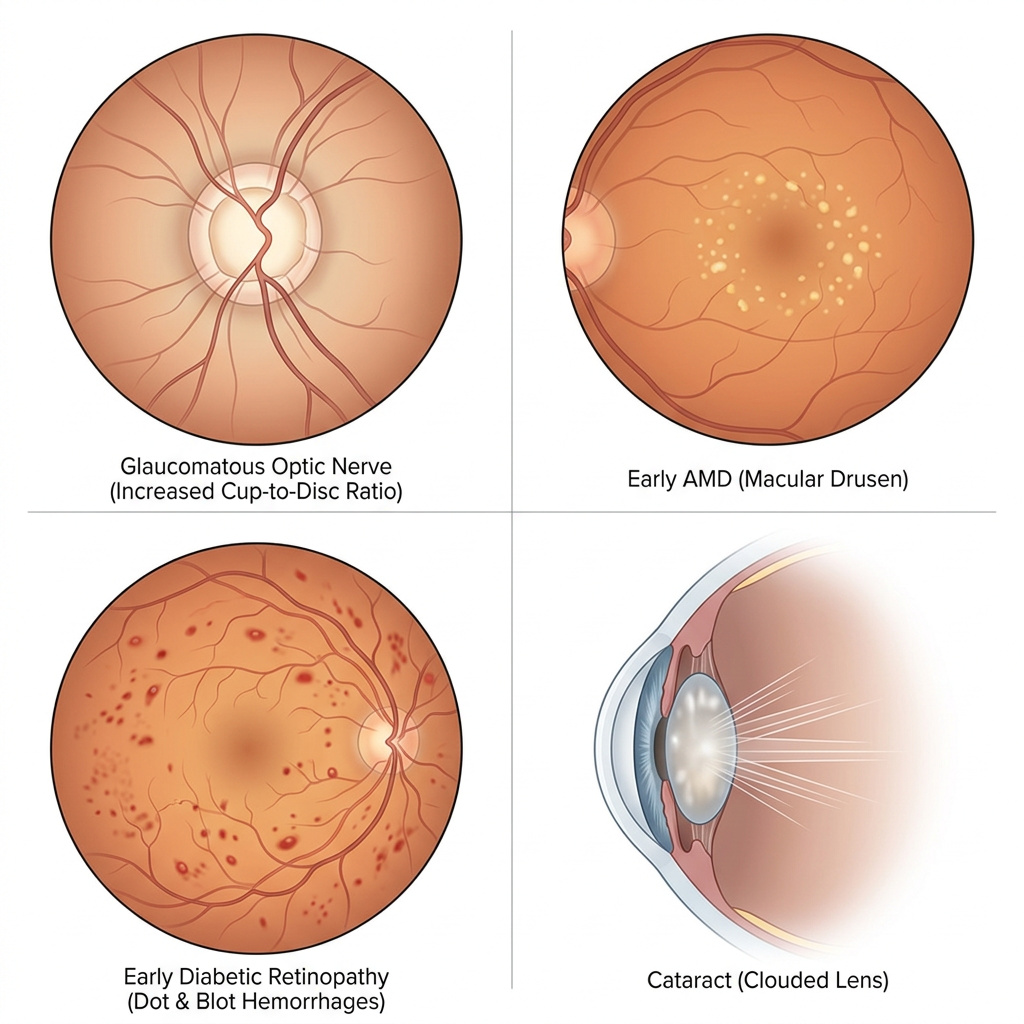
Glaucoma is the second leading cause of blindness worldwide, and the reason it earns the nickname “the silent thief of sight” is precisely what makes early detection so urgent. It damages the optic nerve progressively and almost always painlessly, stealing peripheral vision so gradually that patients do not notice until 40 to 50% of that vision is permanently gone. There is no treatment that restores vision lost to glaucoma. What we can do with eye drops, laser, or surgery is halt or slow further damage. Every year of earlier detection is a year of preserved peripheral vision. We look for elevated or asymmetric eye pressure, optic nerve cupping, nerve fiber layer thinning on OCT, and visual field defects. No single finding is definitive in isolation; glaucoma diagnosis is a clinical synthesis of multiple data points, which is one of the reasons a thorough exam matters.
Age-related macular degeneration is the leading cause of vision loss in adults over 50 in the United States. The macula is the central portion of the retina responsible for sharp, detailed, color vision: reading, driving, recognizing faces. When AMD advances, those abilities degrade in ways that are devastating to quality of life and independence. Dry AMD, the more common form, progresses slowly and can be partially managed with AREDS2 nutritional supplementation once identified. Wet AMD, characterized by abnormal blood vessel growth beneath the retina, can cause rapid central vision loss and requires prompt treatment with anti-VEGF injections, with outcomes that are substantially better when treatment begins early. We look for drusen deposits, pigmentary changes in the macula, and retinal fluid on OCT. This is a condition where annual retinal photography is particularly valuable because the early changes are subtle and comparative documentation makes them visible.
Diabetic retinopathy is the leading cause of blindness in working-age adults in the United States, and approximately 30% of people with diabetes have some degree of it, many of them unaware. High blood sugar damages the microvasculature of the retina, producing microaneurysms, dot and blot hemorrhages, hard exudates, and eventually macular edema and neovascularization. Early diabetic retinopathy has no symptoms and is highly treatable. Advanced diabetic retinopathy can cause sudden, severe, irreversible vision loss. This is the condition that most reminds me why annual exams for diabetic patients are not optional. Finding retinal changes in a patient who did not know they were diabetic is one of the most impactful interventions an optometric exam can produce.
Cataracts affect more than half of Americans by age 75, and their detection is part of every slit lamp examination I perform. We are grading the type of opacity, whether nuclear, cortical, or posterior subcapsular, and assessing its impact on functional vision. Modern cataract surgery is one of the safest and most successful procedures in all of medicine, with outcomes that are excellent when timing is appropriate. Monitoring progression allows us to time that referral precisely, rather than waiting until the cataract significantly impairs daily life.
Retinal tears and detachments represent the acute end of the retinal spectrum. A retinal tear found during a dilated exam in an asymptomatic patient can be treated with a brief in-office laser procedure that welds the retina back to its underlying support tissue, preventing detachment. Once detachment occurs, the required surgery is more complex, recovery is longer, and even with successful repair, full visual recovery is not guaranteed. The peripheral retina, the area most likely to tear, is precisely the region that is only visible with full dilation. This is why I repeat to every patient: please do not decline the dilation.
Vision Screening vs. Comprehensive Exam: Not Even Close
This distinction frustrates every eye care professional I know, and it needs to be stated as directly as possible: a vision screening is not a comprehensive eye exam. They are not interchangeable. They do not answer the same questions. And confusing one for the other has real consequences for patients who believe they are covered when they are not.
A vision screening, whether at a school, a DMV, an employer health fair, or a pediatrician’s office, takes 5 to 10 minutes and answers one question: can you see letters on a chart at 20 feet right now? It does not measure eye pressure. It does not examine the retina. It does not assess the optic nerve or detect macular changes. It does not look for muscle imbalance, corneal disease, lens opacity, or the dozens of structural and vascular findings that a comprehensive exam evaluates. Research shows that vision screenings miss approximately 75% of vision problems in children. In adults, they detect virtually zero cases of ocular disease.
A child can pass a school vision screening with 20/20 distance acuity and simultaneously have significant farsightedness causing headaches and reading fatigue, a convergence insufficiency affecting comprehension, early myopia that will progress rapidly if unmanaged, or a subtle muscle imbalance that is affecting academic performance. An adult can pass a DMV screening and have early glaucoma actively stealing peripheral vision, diabetic retinopathy developing in their retinal vasculature, or a retinal tear waiting to progress to detachment. The screening caught none of it, because the screening was not designed to look for any of it.
Passing a vision screening means you can see at 20 feet today. It means nothing about the health of your eyes, the integrity of your retina, the status of your optic nerve, or your risk for vision-threatening disease. That is what a comprehensive exam is for, and why there is no substitute for it.
How Often Do You Actually Need an Exam?
The honest answer is: it depends on your age, your risk factors, and your current eye health status. Here is the framework I use with my own patients, based on the American Academy of Ophthalmology’s 2025 Preferred Practice Pattern guidelines and the American Optometric Association’s recommendations.
For infants and young children, the AOA recommends a first comprehensive eye exam between 6 and 12 months of age, earlier than most parents realize. A second exam between ages 3 and 5, and then annual exams from school age through age 17. The reason for this frequency during childhood is that the visual system is actively developing, and conditions like amblyopia (lazy eye), strabismus (eye misalignment), and significant refractive error can permanently impair visual development if not identified and addressed during the window when the visual system is still responsive to treatment. School screenings, as I have described, are not adequate substitutes for this monitoring.
For adults aged 18 to 39 without risk factors, the AAO recommends a comprehensive exam every 5 to 10 years, though in practice, anyone wearing glasses or contact lenses should be seen annually for prescription monitoring and contact lens health evaluation. Adults with risk factors for glaucoma, including a family history of glaucoma, African or Hispanic ancestry, diabetes, or elevated eye pressure, should be examined every 2 to 4 years even before age 40.
At age 40, every adult should have a baseline comprehensive eye exam regardless of symptoms or prior eye health history. This is the age at which presbyopia typically begins, at which glaucoma risk begins to climb meaningfully, and at which the early signs of macular degeneration and other age-related conditions become clinically relevant for the first time. From 40 to 54 without risk factors, the AAO recommends every 2 to 4 years. From 55 to 64, every 1 to 3 years. At 65 and older, every 1 to 2 years.
These are minimums for low-risk individuals. If you have diabetes, the recommendation is annual dilated exams from the time of diagnosis. Type 1 diabetics five years after onset, Type 2 diabetics at diagnosis and annually thereafter. If you have a diagnosed eye condition such as glaucoma, macular degeneration, diabetic retinopathy, or any condition under active monitoring, exam frequency is determined by your specific disease status and is typically more frequent than the general schedule above. My standing recommendation to the majority of my adult patients, particularly those over 40, is annual exams. The incremental cost of a yearly exam is small relative to the cost, financial, functional, and emotional, of a disease that advanced undetected between biennial visits.
What to Expect at Your Next Visit
If it has been a while since your last comprehensive exam, or if you have never had one, here is a practical guide to what your visit at The Eye Care Center will look like and how to get the most from it.
Plan for 60 to 90 minutes, particularly if this is a new patient visit or if dilation and advanced imaging are indicated. Bring your current glasses or contact lenses and a list of any medications you are taking, including over-the-counter supplements. If you have had prior eye exams elsewhere and can obtain those records or bring old glasses, the prescription history is useful context. If there is a family history of glaucoma, macular degeneration, or diabetes, tell us, as it changes what we prioritize.
If you will be dilated, plan to have someone drive you home or arrange transportation. Dilation affects near vision and light sensitivity for 2 to 4 hours, and while many patients drive comfortably after dilation, it is worth planning for. We will discuss whether dilation is indicated at your visit. In most cases, for a complete first exam or an annual exam for patients over 40, I recommend it. The 20 minutes of inconvenience is worth the 60% additional retinal visibility it provides.
Bring any questions you have about symptoms you have noticed, things you have read, concerns about your children’s vision, questions about specialty lens options, or anything else. A comprehensive eye exam is a clinical conversation, not just a series of tests. The information exchange goes both ways, and I would rather spend an extra ten minutes in the exam room answering questions thoroughly than have a patient leave without the information they needed to make good decisions about their eye health.
Your Vision and Your Health Are Worth an Hour a Year
A comprehensive eye exam at The Eye Care Center is not just about updating your prescription. It is an annual health evaluation that protects your vision, monitors your eye health, and screens for systemic conditions that your eyes may reveal before any other part of your body does. We have three convenient locations in the Chicago suburbs, open six days a week, with a team that will take the time to explain exactly what we are finding and why it matters.
Schedule your comprehensive eye exam online or call us at 1-888-899-0816. We are in Addison (630-543-0607), Burbank (708-599-0050), and Willowbrook (630-969-2807). Hours: Monday through Thursday 10am–6pm, Friday 10am–5pm, and Saturday 9am–2pm.
Frequently Asked Questions
How long does a comprehensive eye exam take?
A comprehensive eye exam at The Eye Care Center typically takes 45 to 90 minutes, depending on whether advanced imaging is indicated and whether dilation is performed. New patients and patients whose exams include OCT imaging, visual field testing, or retinal photography should plan for the full 90 minutes. Returning patients with no significant changes and no advanced imaging may be seen in closer to 45 to 60 minutes. We recommend budgeting the full 90 to avoid feeling rushed.
Do I really need my pupils dilated every year?
For most patients over 40, and for any patient with diabetes, a family history of retinal disease, or an existing eye condition, yes. Dilation expands our view of your retina from approximately 35% without dilation to 90 to 95% with it. The peripheral retina, the area most prone to tears, detachments, and certain other conditions, is only accessible with a dilated pupil. The inconvenience of light sensitivity and blurred near vision for a few hours is real, but so is the clinical significance of what we can and cannot see without it.
What is the difference between an eye exam and a vision screening?
A vision screening tests whether you can read letters on a chart at 20 feet. A comprehensive eye exam evaluates your prescription at multiple distances, measures eye pressure, examines every structure of the eye under magnification, dilates the pupil to examine the full retina, and screens for over 270 eye and systemic health conditions. Research shows vision screenings miss approximately 75% of vision problems in children and detect virtually zero cases of eye disease in adults. Passing a screening does not mean your eyes are healthy. It means you can see clearly at that moment.
Can an eye exam really detect diseases outside the eye?
Yes, and this is one of the most clinically important aspects of a comprehensive eye exam. Your eyes are the only place in the body where blood vessels, nerve tissue, and central nervous system tissue can be directly visualized without invasive procedures. During a dilated exam, I can identify retinal changes consistent with diabetes, hypertension, elevated cholesterol, autoimmune disease, neurological conditions, and certain cancers. Many of these findings appear in the eye before they produce symptoms elsewhere in the body. I have personally referred patients to primary care following eye exam findings that led to new diagnoses of Type 2 diabetes, elevated intracranial pressure, and hypertension.
How often should children have eye exams?
The American Optometric Association recommends a first comprehensive eye exam between 6 and 12 months of age, a second exam between ages 3 and 5, and annual exams from school age through age 17. This frequency reflects the fact that the visual system is actively developing during childhood, and that conditions like amblyopia, strabismus, and progressive myopia are most effectively treated when identified early. School vision screenings are not an adequate substitute for annual optometric exams. They miss the majority of clinically significant vision problems in children.
What should I bring to my eye exam?
Bring your current glasses and contact lenses (including the box or prescription information if you have it), a list of all current medications including supplements, your insurance card, and any prior eye exam records if you are a new patient. If you have a family history of glaucoma, macular degeneration, diabetes, or other hereditary eye conditions, be prepared to discuss it, as that history directly influences what we prioritize during the exam. If you are being dilated, arrange for a driver or plan to wait the 2 to 4 hours for full visual recovery before driving.
What does it mean if my eye doctor recommends OCT imaging?
OCT (Optical Coherence Tomography) creates high-resolution cross-sectional images of your retinal layers at a resolution of 5 microns, approximately one two-hundredth the width of a human hair. It allows us to detect structural changes in the retina and optic nerve, particularly early signs of glaucoma, macular degeneration, and diabetic macular edema, at a stage when they are not yet visible in a standard clinical exam and have not yet produced any symptoms. OCT is not cause for alarm. It is a precision tool for earlier and more accurate diagnosis, and it is part of how we protect your long-term vision proactively rather than reactively.